Living with inverted nipples can bring up a mix of feelings – curiosity about why it happens, frustration with how it looks, or even worry about how it might affect breastfeeding. For many, it’s something they’ve dealt with for years, unsure if it can be fixed.
In Baltimore, Maryland, Dr. Ronald Schuster has helped many people address this common breast condition. Using advanced techniques, he can correct inverted nipples while aiming to preserve sensation and, when possible, support breastfeeding ability. Dr. Schuster’s goal is to help you feel reassured and ready to explore your options.

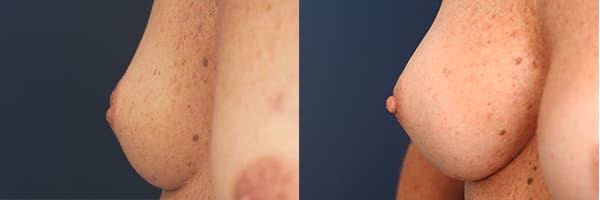
Inverted Nipples - Before & After
Click the image to view the full gallery.
Levels of Severity
In 1999, a grading system was described by Han and Hong. It is still used today to describe the severity of inverted nipples. In addition to being able to classify a patient’s condition, it helps to predict the success of different treatments. There are three grades:
Grade I
In Grade I, the inversion is mild. The nipple can easily be everted with gentle pinching and can maintain an everted position for a short time while the areola contracts.
Surgical correction of this grade can usually be accomplished with just a buried suture at the base of the nipple. You should be able to keep sensation and the ability to breastfeed.
Grade II
Grade II inverted nipples can also be manually everted, but it takes a lot more effort. The nipple does not stay everted and quickly becomes inverted when released. Usually, the ducts are not too short, but they are being pulled downward by the fibrous tissue.
The ducts can be released by dividing the deep fibrous tissue. Adding the buried suture maintains the everted position and completes the procedure. We can typically maintain sensation and the ability to breastfeed, but it is not guaranteed.
Grade III
Grade III is the most severe. The nipple cannot be everted manually. There is a lot of fibrous tissue that keeps the nipple inverted, and the ducts might be physically shortened. This is the most difficult grade to successfully treat.
There have been many types of procedures designed to correct Grade III inverted nipples. They all have certain things in common. They divide the fibrous tissue, keep the nipple everted after surgery with a traction suture, and add tissue into the nipple.
Adding tissue helps to add bulk, which is lacking once the nipple is everted. The tissue usually comes from dermal-fat grafts taken from an inconspicuous area (usually groin).
Patient Testimonial
"I had a wonderful experience with Dr. Schuster and his entire staff. Very professional, personable and helpful. My procedure went very smooth and I am very pleased with my results. I would highly recommend!"
How Dr. Schuster Performs Inverted Nipple Surgery
For severe inverted nipples (Grade III), Dr. Schuster uses a technique involving careful dissection under magnification. This method, first described by Chen et al. in 2007, allows for precise correction through a tiny incision at the base of the nipple.
During the procedure, Dr. Schuster carefully releases the tight tissue that’s causing the inversion while protecting the milk ducts, nerves, and blood vessels. To provide support and shape, a small piece of skin and fat are taken from a discreet area, like the groin, and placed inside the nipple. Two stitches secure the base, and a protective bandage is worn for one week to maintain the correction.
Although this method takes more time and precision, Dr. Schuster believes it offers the best chance for long-term success while preserving sensation and breastfeeding ability. In extreme cases dividing some of the ducts can give a better result and will be discussd beforehand by Dr. Schuster.
What Can I Expect From Recovery?
The surgery is performed on an outpatient basis under IV sedation. It is not painful after surgery. A slightly bulky bandage is worn for a week. Light protection is needed for six weeks after surgery. Exercise can be resumed three weeks after surgery.
Why Correct Inverted Nipples?
Inverted nipples are really just a cosmetic issue. Inverted nipples can make it difficult but not impossible to breast feed. A consultation with a special lactation nurse is helpful to learn how to breast feed or pump even if you have inverted nipples. Surgical correction should not be done for the sole purpose of breast feeding since a risk of the surgery is the inability to breast feed. Anectodedly many patients have reported backthat they were in fact able to breast feed after surgical correction. Most patients simply feel self-conscious about how it looks and want to feel more feminine and at ease with their body. Fixing inverted nipples can solve these issues, helping you feel more comfortable and free to live without worrying about it anymore.
Choosing Dr. Ronald Schuster
Dr. Ronald H. Schuster is a board-certified plastic surgeon based in Baltimore, MD. He completed his medical training at the University of Maryland, followed by a general surgery residency at Sinai Hospital and a plastic surgery fellowship at Washington University’s Barnes Hospital. He also served as chief of the Plastic Surgery Division at Northwest Hospital Center and now leads his private practice.
Dr. Schuster specializes in a wide range of cosmetic procedures for the face, breast, and body, as well as non-surgical treatments like laser resurfacing and BOTOX® therapy. Dr. Schuster’s thoughtful approach and proven skill make him a trusted choice for patients seeking cosmetic surgery.
Frequently Asked Questions
The inverted nipple correction procedure usually takes around a 1 1/2 half hours total. If it is only a minor correction, the operation can take just an hour.
No, the procedure itself is not painful. Before an inverted nipple procedure can take place, patients are given a local anesthetic. You may feel slight discomfort from the anesthetic, but you will not feel anything from the procedure. Be sure to consult the surgeon regarding the anesthesia before the operation begins.
Recovering from the initial procedure and returning to your semi-normal routine can take about a week or two. For a full recovery from an inverted nipple procedure, it can take up to six weeks. However, recovery can potentially take longer, depending on your health.
Inverted nipple surgery is usually a safe procedure, but it does have a few risks you need to consider.
The risks of inverted nipple surgery include the following:
- Bleeding
- Contracting an infection in the treated area
- Asymmetry
- Scarring
- Changes in nipple sensation
- Reoccurring nipple inversion
- Undesired aesthetic results
- Inability to breastfeed
Dr. Ronald Schuster will go over these risks during your consultation with him. He will go over your medical history, habits, and past surgical complications to see whether or not you are a suitable candidate for inverted nipple surgery.
The ideal candidates are patients who are unhappy with the appearance of their inverted nipples. Patients should be in relatively good health, not pregnant or currently breastfeeding, and have realistic expectations regarding the procedure.
Inverted nipples can be caused by shortened milk ducts, tight connective tissue, or fibrous tissue beneath the nipple. In some cases, it may be a genetic trait present from birth. Hormonal changes, aging, trauma, or certain medical conditions can also contribute to nipple inversion.
While the goal of surgery is to provide a long-lasting correction, there is a chance that inverted nipples can return. The likelihood depends on factors such as the severity of the condition, your healing process, and post-surgical care. Grade III cases have a slightly higher risk of recurrence compared to milder grades.
The scars from inverted nipple surgery are typically small and well-concealed at the base of the nipple. Over time, they usually fade and become less noticeable.
Insurance does not cover inverted nipple surgery as it is usually considered a cosmetic procedure. However, if the condition is causing functional issues, such as difficulty breastfeeding, some insurance providers may offer partial coverage. It's best to check with your provider for specific details.
Schedule a Consultation
To learn more about how Dr. Schuster treats inverted nipples, please call our office at 410-902-9800 to book a consultation. Dr. Schuster will review your specific condition, explain the surgical technique, and discuss what results you can realistically expect from the procedure.